HOPEFUL SUCCESS FOR IDIOPATHIC PULMONARY FIBROSIS
 By
Dr. Nick P. Trifelos, M.D.
By
Dr. Nick P. Trifelos, M.D.
August
21, 2014
NewsWithViews.com
A PERSONAL PERSPECTIVE
ABSTRACT
This is an account of my experience after being diagnosed with idiopathic pulmonary fibrosis in November 2009. This is a fatal disease with a 3-5 year life expectancy from the date of diagnosis, maybe a little longer with supplementary treatment. The purpose of this report is to bring attention to the value of proteolytic enzymes in dealing with idiopathic pulmonary fibrosis.The paper describes the success I had combating the disease after discovering the potential and use of proteolytic enzymes, changing the recommended treatment model to facilitate a clinically acceptable respiratory lifestyle and hopefully continue these changes for the duration until a cure is found.
The Problem
Idiopathic pulmonary fibrosis (IPF) is a well-known condition which is a fibroproliferative event causing scarring of the interstitial areas of the lungs, crushing the alveoli ultimately causing the inability to breathe. The lung cells themselves (alveoli) are essentially unaffected but are compressed by the surrounding interstitial scar tissue. This is a fatal condition. The estimated life expectancy from the date of diagnosis is 3 to 5 years, sometimes a little longer depending on the response to supplementary treatment.
There is an estimated 200,000 cases in the United States with 50,000 new cases and 40,000 deaths each year. There are multiple causes of pulmonary fibrosis including airborne toxins, certain lung diseases including pneumonia, radiation exposure, certain chemotherapeutic agents,some antibiotics and GERD (acid reflux) to name a few, but the specific cause of idiopathic pulmonary fibrosis (IPF) has yet to be determined. An immune problem has been considered but immune suppressive medications have thus far not been effective. Recent attention has been aimed at fibroblast dysfunction at the molecular level and this shows early promise for definitive answers.
Treatment has been basically ineffective. N-acetylcysteine (NAC) primarily as an antioxidant and anti-inflammatory has been used with little response. Steroids may be effective in 20% of the patients but only for a short period. Pirfenidone, approved in Canada but at the time of this writing not yet in the United States, shows some promise in combating this disease especially in mild to moderate IPF. A small molecule drug that inhibits TGF-B, a fibrogenic mediator reducing fibroblast proliferation, is the promising component of the drug. It also reduces inflammation by reducing the life of mediator TNF-A. A new study published by investigators at the University of Alabama Birmingham reveals a new discovery of the pathway that leads to fibrosis and scarring of the lungs. They call this mechanosensitive signaling of myofibroblasts.[15] They explain this in their article as follows “myofibroblasts are cells responsible for wound healing in the body. In healthy tissues, myofibroblasts assist with wound repair then die in a pre-programmed process known as apoptosis. Fibrosis involving the lungs or other organs occurs when fibroblasts fail to undergo apoptosis resulting in a persistent repair process”. They found that a protein called Rho-kinase (ROCK) may cause the failure of apoptosis causing the continued fibrosis resulting in the disease. Cells are known to respond to certain mechanical cues and ROCK was the pathway to prevent apoptosis, but, by the same token this may be the window to impede the ROCK pathway providing significant treatment. This opens the door for research in existing and new ROCK inhibitors. Fasudil, a known ROCK inhibitor and vasodilator used for stroke victims and effective against pulmonary hypertension has recently been taken off the market because of the significant side effects.
Recent attention has been directed to the use of nintedanib, a triple tyrosine kinase inhibitor affecting 3 primary targets: Platelet derived growth factor (PDGF), vascular endothelial growth factor (VEGF) and basic fibroblast growth factor (BFGF). Presently, it is in late control trials for the vascular VEGF treatment of cancer facilitating angiogenesis inhibition precluding the neo-vascularity necessary to feed the tumor with resultant“starvation” (lack of oxygen) and death of the tumor. In addition it was recently found to have a profound improvement of IPF because of a significant suppressive effect on the fibrous growth(FGFR) with an impressive enough potential to cause the FDA to put nintedanibon“breakthrough therapy” status assuring control trials start early. This may work in tandem with the work being done by Dr. Thannickal, time will tell. A variety of research is being done in many universities but is still in early stages and results are yet to be determined. Unfortunately patients presently continue to have a downhill course, oxygen offers some relief until death occurs close to the predicted 3-5 years.
Discovery of the Affect of Proteolytic Enzymes on IPF
I have IPF initially diagnosed in December 2009 which I refused to believe because I was breathing well with only increased shortness of breath (SOB) on climbing a flight of stairs. However in the summer of 2011 my breathing became increasingly labored and by September it became quite severe. I developed all the symptoms typical of the disease; I was moving slower; I could barely keep my eyes open; I had severe tightness in my chest and was preparing to use oxygen for my last days. My cough (typical of the disease) occurred every 9 seconds (by the clock) and all the symptoms were progressing as expected. I decided to search the internet to find relief for the cough and in so doing stumbled on to an “alternative treatment for IPF” used by nutrition companies. The product being promoted was proteolytic enzymes. These were non-human enzymes used for over 50 years specifically to clear arteries from the sludge but were also found to have additional properties; namely anti-inflammatory action, mild anticoagulation effects and a general fibrinolytic effect throughout the body, including the lungs. They are reported to breakdown scar tissue (fibrinolytic action) to its component parts which are subsequently removed from the body by the bowels, urine or perspiration.
Originally these enzymes were thought to be specific targeting an exact protein substrate using the key-lock system, however, research shows these enzymes are diverse and specificity is true only in part. People on these enzymes primarily for vascular cleansing who also had IPF were found to significantly improve in their breathing. I discussed their use with my pulmonologist and medical colleagues and all had reservations as to their use, but when one is in a terminal position as I was, most will do what they can to reverse it. I called the companies, talked to their spokesmen, read their testimonials and started on the proteolytic enzymes. I noticed improvement in 2 weeks, normal breathing within 8 weeks and with only minor limitations I was living a normal life. Virtually all who reported on their results had some improvement, some better than others and in my case I had a positive response apparently very quickly. They do not cure IPF but apparently suppress and restrain its progress.
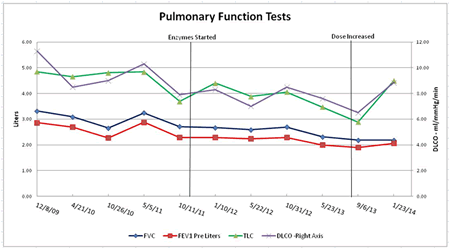
I have been taking these for over 2 years. The table shows a history of my pulmonary function studies (PFTs) from the beginning of my diagnosis at 12/8/2009. The 4 studies used were FVC (Forced Vital Capacity), FEV (Forced Expiratory Volume), TLC (Total Lung Capacity) and DLCO (Diffuse Capacity).The FVC, FEV1 and TLC are measured in liters. The DLCO is measured in ml/mmHg/min.

Table
The graph shows a relatively sharp decline in all studies except for the TLC in April and October 2010. I began taking the enzymes the last week of October 2011 and in January 2012 two studies improved (TLC and DLCO) one was unchanged (FEV1) and one slightly declined (FVC). The subsequent studies then showed a decline but at a slower rate suggesting the enzymes are effective but are incomplete with the present treatment methodology. The most recent studies (January 2014) show improvement. The explanation for this is addressed later in the article. Symptomatically, I was stable for about 18 months when dyspnea again recurred in the summer of 2013 as could be predicted by the PFTs which continued to decline from the progressive scarring.
There are certain pulmonary vulnerabilities with this disease. Aside from the increased inflammation and mucous, infection with minimal external exposure is prominent, especially interstitial pneumonia. I started periodic ciprofloxin alternating with Keflex as a preventive measure which was effective. With the onset of the recent episode of dyspnea and after discussion with my pulmonologist, we decided to change the antibiotic regimen to Zithromax 250 mg. daily. Also, because of the research I did on this disease and treatment by these enzymes I increased the dosage of one of the enzymes 3 fold. The results were very positive. I am back to breathing as I did before the change. In my mind this raises the question as to what is the appropriate dosage for the most effective action by these enzymes for this disease. On questioning the manufacturer the present dose recommended is used primarily for the cleansing of arteries. It appears different doses may be necessary for different problems.
The medical profession has not adopted the use of proteolytic enzymes for IPF treatment most likely due to lack of controlled trials. I, as a physician agree that claims can be made but it is necessary to be sure the claims are true. Partial studies have been done in Japan and Europe but these generally lacked the specifications required by American Medical standards.
The Value of Proteolytic Enzymes
The reason I am enthusiastic about these enzymes and felt obligated to write this paper is because as a result of these enzymes my predicted demise changed to a possibility that IPF might have little or no influence on my life expectancy. In addition, once one investigates these proteolytic enzymes a whole new panorama of information opens as to the prevention and treatment of many human diseases, IPF being only one. The effective use of proteolytic enzymes in IPF and other diseases will raise many eyebrows but after reading the experiences of other professionals using these enzymes as well as my personal experience I feel that open minds are in order.
Time does not permit an in-depth review of proteases, one can find this in the hundreds of articles written. Two specific papers recommended to the interested reader are Future Research Direction in IPF from the workshop by the National Heart, Lung and Blood Institute and Proteases: Multifunctional Enzymes in Life and Disease by Lopez-Otin and Bond. However, touching a few highlights will hopefully generate enough curiosity to stimulate a second look and pursue further research. As stated earlier, once thought of as simple enzymes used to breakdown scar tissue which is still their primary function, now we realize their diversification. They range from simple enzymes with a specific target substrate to complex multifunctional machines whose actions are variable and multiple. Many enzymes are non-specific for substrates attacking them in an unorthodox manner adapting to whatever measures are necessary to complete their function. Conversely, they can work in tandem facilitating a symbiotic pattern with each other to the complete lyses of a complex substrate. They can also create peptide bonds in certain circumstances. Enzyme inhibitors are one of the main destructive forces of these enzymes but some can change their sensitivity to endogenous inhibitors and continue to remain effective. They can act in complex networks of protein groups that interact to form the “protease web” that provides multifunctional protease activity.[2] The list of their functions too numerous to mention here continues and can be found in the literature.
Because of these diverse functions enzymes are known to control multiple biological processes in the body. According to Lopez-Otin and Bond proteases (a) regulate the fate, localization and activity of many proteins, b) modulate protein-protein interactions, c) create new bioactive molecules, d) contribute to the processing of cellular information and e) generate, transduce, and amplify molecular signals. As a result of these functions, proteases influence DNA replication and transcription, cell proliferation and differentiation, tissue morphogenesis and remodeling, heart shock and unfolded protein responses, angiogenesis, neurogenesis, ovulation, fertilization, wound repair, stem cell mobilization, hemostasis, blood coagulation, inflammation, immunity, autophagy, senescence, necrosis and apoptosis.[2] Basically they affect almost all or all of the necessities for development and survival of life. Knowing this, one can imagine the value in prevention and treatment by understanding and controlling the activity and action of these enzymes against diseases and chronic conditions affecting mankind.
Interest in the United States
Although treatment using proteases has been used extensively in Europe and Asia for many years, there was little interest in the U.S. until William Kelly DDS pioneered work on cancer and degenerative diseases but was met with a significant negative response. Upon his death Drs. Nicholas Gonzalez and Linda Issacs (both MDs) picked up the torch pursuing alternative medicine (enzyme therapy) for treatment of pancreatic cancer. At first there was much resentment and major controversy by the medical profession regarding this approach especially since the initial results were not favorable. However, now it is being funded for research by the N.I.H. (National Institutes of Health) and according to Dr. Gonzales because of the popularity of alternative therapy in the 1990’s more than two dozen medical schools and hospitals established centers of alternative medicine in an attempt to coordinate this with conventional treatment.
Dr. Jim Howenstine, M.D’s. article How Systemic Enzymes Work to Cure Disease presents an excellent synopsis of the manifestations of these enzymes. On reviewing the articles of those with many years of experience in treating patients, one uncovers many interesting facts. We can account for about 3,000 plus enzymes but estimate there to be 30,000 in existence, new ones being discovered on a regular basis. Normally we are born with a full complement of proteolytic enzymes which circulate performing their functions including aiding the immune system to handle invaders (viruses, bacteria, cancer cells). Consequently in our youth for the most part we stay healthy protected from the chronic diseases seen later in life. There are exceptions of course namely childhood diseases due to various causes including the lack of enzymes but percentage wise the diseases start in the mid-thirties to forties. According to Howenstine, proteolytic enzyme production begins to diminish at age 27 and by age 35 is significantly reduced which is about the time the chronic diseases and illnesses of older age begin and as time passes the diseases increase. One can use a cause and effect argument stating that these illnesses occur because of the lack of proteolytic enzymes and on studying and understanding their effect and performance, the argument for the enzymes carries great validity. The treatment for cancer can act as an example. We all know cancer cells circulate in our bodies from birth but are for the most part destroyed. According to the authors, all cells are protected by a fibrin coat but the cancer cells are protected by a coating up to 15 times thicker than normal cells. In our youth we generally have adequate numbers of enzymes to dissolve the cancer coating and allow our immune system to attack and destroy the cancer, but as the numbers of enzymes lessen, the opportunity for these malignant cells increases and eventually create a problem.[3] This scenario can also apply to many illnesses possibly because the inflammation (the first line of defense) becomes excessive leading to various illnesses. Aging may also be related to the subtle fibrin involvement of internal organs and systems.
Use of Enzymes
Some say that non-human enzymes may not be efficient in humans because of stomach acidity (Drs. Mary Campbell and Shawn Farrell), however, these enzymes are now enteric coated and pass into the intestines unaffected. They are divided into digestive and systemic classifications. Actually, they are the same enzyme, the difference being where they perform their function; digestive if they are active in the stomach and systemic when they pass into the intestine and are absorbed and act in the circulation. Therefore, it is important to take them on an “empty stomach”, timing being critical, since their action begins immediately on contact with fibrin. The manufacturer recommends waiting at least 2 hours after a meal for the stomach to empty before taking the enzymes and then, wait 1 hour for them to pass into the intestines before eating. According to previous research they can be taken in quite large amounts (well over 100 capsules daily) without significant side effects except for the 2 previously mentioned (anti-inflammatory and mild anticoagulation). Occasional skin rash and muscle aches have been reported but disappear when the enzyme is stopped. The original use by the nutrition companies was to “clear the sludge” from the arteries preventing arteriosclerosis but the list of benefits and positive results of enzymes on healing various diseases including cancer is long and can be found in many articles.
For treating my IPF I am taking 2 of these non-human enzymes, serrapeptase and nattokinase purchased from Pivotal Health Products (http://www.pivotalhealth.info/). They are manufactured by AST Enzymes (http://www.astenzymes.com/). Commercially they are sold as Serra RX containing only serrapeptase and Serracor-NK containing both serrapeptase and nattokinase along with additional enzymes –Bromelain, Papain, Lipase, Rutin, CoQ10 and others. The serrapeptase enzyme is isolated from the microorganism Serratia found in the intestines of silkworms and used to free the moth from the fibrous cocoon. Natto, a popular Japanese food is made from fermented soybeans by using the bacteria bacillisnatto creating many enzymes, the most important being nattokinase. The maximum dose suggested by the manufacturer is three (3) caps of Serracor–NK and 2 caps of Serra RX three (3) times daily on an empty stomach (as previously described).The fibrinolytic action of these enzymes is measured in FUs (fibrinolytic units) although SUs (serrapeptase units) and IUs (international units) have been used by certain individual companies but all apparently are the same unit. The serrapeptase capsule contains 80,000 FUs. The nattokinasecapusule has no FU measurement on the label. Initially this worked well for me treating my IPF.
My Plan and Results
Much has yet to be evaluated in this area and I feel that dosage is a main determinant. It is not a question of whether proteases work against IPF, they worked for me. The question remains on how high a dosage can be ingested without untoward effects to reach the level of fibrotic reversal. According to those with experience in treating patients, the upper limit of dose is higher than the currently recommended doses by nutrition companies. When my second set back started (June 2013) I increased the SerraRX (serrapeptase) to first 4 then 6 caps 3 times daily keeping the nattokinase unchanged. Within 3 weeks my breathing again became normal with no side effects. One can equate this as a force of 100 coming on with only a force of 40 to counteract it, you’ve slowed it down but not enough to completely stop or reverse it. I continued to increase the enzymeserrapeptase to 33 capsules daily maintaining the nattokinase at 9 capsules to a total of 42 capsules per day with no side effects. The most recent PFT studies (January 2014) show improvement for the first time since the onset of the enzymes with the FVC unchanged and improvement of the other 3 (FEV1, TLC, DLCO). Although this is a positive indicator, it may be too early to draw any conclusion. There are many variables involved not the least of which is that these studies were conducted on a different machine. Follow up studies in 4 months should answer many questions. My plan is to continue the present course of treatment, increase the enzyme dosage as necessary to maintain normal breathing and begin the Pirfenidone when it becomes available to stop the fibrotic aberration at its source.
At the workshop of the National Heart Lung and Blood Institute (NHLBI) on an extensive review of present and future research on IPF their conclusion was to proceed with a 2 pronged attack. The first being to attack the problem at its origin at the molecular fibroblast level and it appears Pirfenidone inhibiting the TGF-B fibroblast mediator and the most recent research submitted by Dr. Victor Thannickal at the University of Alabama Birmingham regarding the mechanosensitive signaling of myofibroblastsdiscovering the enzyme Rho-kinase as the inhibitor of apoptosis and allowing the fibrotic process to continue with a pathway to find a possible cure along with the potential nintedanib offers is a good start.[16] The second approach is to lyse the fibrotic tissue, to dissolve and remove the scar already in place. Continued research on proteolytic enzymes to perfection may fit and resolve this need.
The experience of one person may not be entirely convincing but one can find many testimonials reiterating the same experience on the internet. Irregardless of the outcome of my personal situation and if the result is not what I’m hoping for based on the declining PFTs suggesting the force of the disease is met with inadequate resistance, it is not because the enzymes didn’t work, they worked for me. I strongly feel it’s because the enzymes haven’t been utilized to their maximum potential suggesting the need for definitive research.
|
|
Again, I want to emphasize that this is a report on my experience in the use of proteolytic enzymes against IPF. I am not alone in this based on the testimonials written by people that used them for this purpose. I am in no way advocating their use at present as definitive treatment but merely suggest a second look at these to undergo the standard acceptable well established requirements to prove or disprove their value. I have also rendered my thoughts and direction to take I feel would maximize their function at the present level. My hope is that these enzymes will be used for their value in the short term and with definitive research may become a part of the established treatment for the future.
STATEMENT
I want it known that I have no financial interest or compensation regarding these enzymes. I pay full price out of pocket for the cost of these enzymes and the preparation of this paper. I consider discovering their action on me a gift and want to pass the message on the same way. --Nick Trifelos MD
© 2014 Nick P. Trifelos, M.D. - All Rights Reserved
BIBLIOGRAPHY
1.
National Heart Lung, and Blood Institute Working Group, Future Research
Directions in Idiopathic Pulmonary Fibrosis. American Journal of
Central Care Med Vol 166 p. 236-246.
2. Lopez-Otin, Bond. Proteases: Multifunctional
Enzymes in Life and Dis., The Journal of Biological Chemistry. Vol.
283 No. 45.
3. Howenstine, James M.D. How
Systemic Enzymes Work to Cure Diseases Part 1 and Part 2. NewsWithViews.com.
4. Barrett AJ, Rawlings ND, Woessner JF. Handbook
of Proteolytic Enzymes 2nd Ed. Academic Press 2003.
5. Southan C. A Genomic Perspective on Human Proteases
as Drug Targets. Drug Discov Today 6:681-688.
6. Ciechanover, A. National Dev. Molecular Cell
Biol. 6, 79-87.
7. Lopez-Otin, Matrisian, LM. National Rev. Cancer,
2007, 7, 800-808.
8. Kuhn C III. Patterns of Lung Repair: A Morphologist’s
View. Chest 99:115-145.
9. Raghu G, Chen Y, Rabinovitch PS. Differential
proliferation of fibroblasts cultured from normal and fibrotic human
lung. Am Rev Respir Dis., 1988;
10. Chapman HA Jr., Allen CL, Stone OL. Abnormalities
in pathways of alveolar fibrin turnover among patients with interstitial
lung diseases. Am Rev Respr Dis 1986: 333; 437-443.
11. Bitterman PB, Rennard SI, Keogh BA, Wewers,
MD, Adelberg S, Crystal RG. Familial idiopathic pulmonary fibrosis.
Evidence of lung inflammation in unaffected family members. N Engl
J Med 1986: 314
12. Proteolytic Enzymes. Wikipedia
13. Enzyme
Inhibitors
14. Hefferon S. What
are Systemic Proteolytic Enzymes and How Can you Benefit from Them.
15. Zhou Y, Thannickal VJ, et. Al. Inhibition of
mechanosensitive signaling in myofibroblasts ameliorates experimental
pulmonary fibrosis. The Journal of Clinical Investigation, March
2013. Vol 123 Num. 3: 1096-1108
16. Antoniu S. Nintedanib (BIBF 1120) for IPF:
a tomorrow therapy? MultidiscipRespir Med. 2012; 7(1): 41.
Nick P. Trifelos, M.D. Biography
Education:
Canton McKinley High School 1953 The Ohio State University - B.S.–Double
Major; Chemistry &Biology 1957 The Ohio State University - M.D.
1962
Training:
Medical Internship-St. Elizabeth Hospital - Youngstown, OH 1962-1963
(Now NE Ohio Medical College) General Surgery Residency –
St. Vincent Hospital - Toledo, OH 1965-1966 (Now Ohio Medical College)
Urology Residency-Ohio State University Hospital 1966-1969 (Co-Authored
publication on Renal Vascular Research)
Military:
U. S. Army Captain-3rd Army, Womack Army Hospital 1963-1965 Ft.
Bragg North Carolina (Started in 3rd Army but attached to 82nd Airborne
Division- While in service was the head of the REM team (Radiological
Emergency Medical Team) – Purpose – first responders
to a nuclear explosion on the East Coast of Carolinas and Georgia)
Practice
(Urology):
Private Practice - Nick P. Trifelos, M.D., Inc. - Newark, Ohio 1969-1999
Licking Memorial Hospital (Primary Hospital) - Chief of Urology
for 27 years; involved with multiple 1969-1996 functions and committees
Also on Staff at: Park Medical Center (Now OSU East) Coshocton Hospital
in Coshocton, Ohio
Professional
Organizations:
American Urological Association 1970–Present North Central
Section of the AUA 1970-Present Ohio Urological Society Charter
Member Central Ohio Urological Association - President 1972-1973
Licking County Medical Society - President 1990-1991 OSMA 1962-Present
AMA 1962-Present Others
Service
Organizations:
Rotary (Paul Harris Fellow) 1974–Present AHEPA (American Hellenic
Education Progressive Association) 1972-1982 Washington, D.C. (Greek
Service Organization started in the late 1800’s to help Greek
immigrants become good productive Americans)
Community:
Board – Newark Health Department 1985-1989 Board – Pine
Seminary 1973-1977 Football Team Physician- Newark Catholic 1972-1992
Founder:
Cooleys Anemia Foundation of AHEPA – Washington, D.C. National
Chairman 1972-1975 Medical Director 1972-1982 Moundbuilders Physician
Association - President 1985-1992 (Purpose - to help doctors with
the business aspects of their practice)
Co-Founder:
Newark Surgery Center 1997 Ohio Kidney Stone Center – Board
Member 1985-1995
Latter Years – Was diagnosed with Idiopathic Pulmonary Fibrosis and presently working on resolving this disease.
Contact
Dr. Trifelos at: n.trifelos.md@gmail.com












 Share
This Article
Share
This Article





